Definition
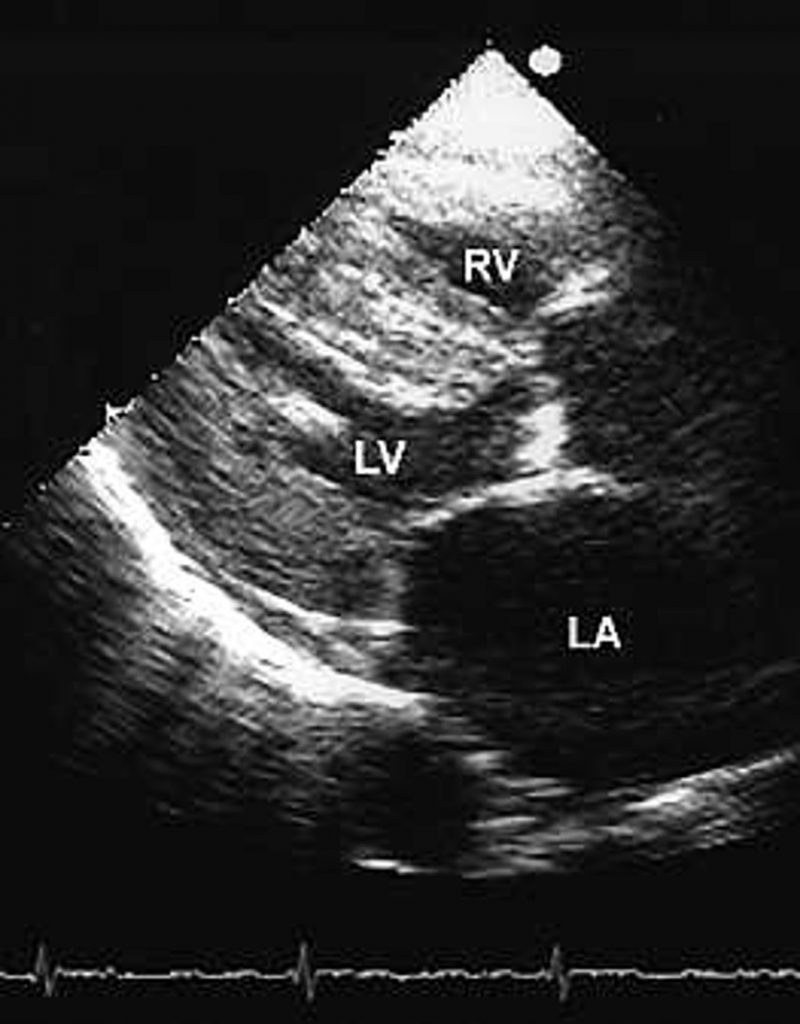
HCM is characterized by asymmetrical hypertrophy of the heart, with a predilection for the interventricular septum, and high degree of myocyte disarray in the absence of hemodynamic stresses sufficient to account for the degree of hypertrophy, and systemic conditions such as amyloidosis and glycogen storage disease, which have been associated with HCM phenocopies. Familial HCM affects an estimated 1 in 500 people worldwide with similar prevalence in males and females.
HCM is the most common monogenic cardiovascular disease as well as the most common cause of sudden cardiac death in young adults. It often has a subclinical course and patients are diagnosed incidentally, nevertheless, a sizable proportion presents with angina, dyspnea, palpitations and syncope. HCM can also lead to exercise disability at almost any age, progress to heart failure with or without preserved ejection fraction, or be complicated by atrial fibrillation (AF) associated with risk of embolic stroke. Sudden cardiac death in HCM is primarily mediated by VF, but asystole and pulseless activity also have been reported. The annual risk of SCA is estimated to be 1% in general HCM population, while those with prior VT, VF or aborted cardiac arrest have 10% annual risk for sudden death and mortality rate of 4.7%. In Obstructive HCM (HOCM) nearly 70% of all deaths are sudden.
Some atypical forms of hereditary HCM (fenocopies) are due to deposit disorders (mutations in PRKAG2, GAA, GLA, LAMP2) . It is important to detect this type of HCM since opportune treatment can avoid the development of permanent heart damage.

Why to perform genetic testing in cases with suspected HCM?
- Novel genetic data and genotype-phenotype correlations studies in HCM have shown important genetic bad outcome risk factors
- To precisely diagnose the cause of the disease. This information has therapeutic and prognostic consequences
- To identify some genetic forms known to provide higher risk of sudden cardiac death
- To detect family members at risk who may need clinical follow up and life style recommendations
- The genetic test in HCM patients is recommended by the ESC Guidelines of HCM management 2014.
Our HCM genetic test short panel
ACTC1, CSRP3, MYBPC3, MYH7, MYL2, MYL3, TNNC1, TNNI3, TNNT2, TPM1.
Our HCM genetic test broad panel
ACTC1, ACTN2, ALPK3, CACNA1C, CSRP3, DES, FHOD3, GAA, GLA, HFE, JPH2, LAMP2, MYBPC3, MYH7, MYL2, MYL3, PLN, PRKAG2, PTPN11, TNNC1, TNNI3, TNNT2, TPM1, TRIM63, TTR.
Important: All our panels can be modified based on the phenotype. Please contact us if you have questions
What to expect from this test: The HCM genetic test has a variable yield of 40-80%. Depends on the HCM morphology, family history and age of onset of the disease.
Recommended Literature
- Long-term Outcomes of Pediatric-Onset Hypertrophic Cardiomyopathy and Age-Specific Risk Factors for Lethal Arrhythmic Events. Maurizi N, et al. JAMA Cardiol. 2018 Jun 1;3(6):520-525. doi: 10.1001/jamacardio.2018.0789.
- Hypertrophic Cardiomyopathy: Clinical Update. Geske JB, et al. JACC Heart Fail. 2018 May;6(5):364-375. doi: 10.1016/j.jchf.2018.02.010.
- Translating emerging molecular genetic insights into clinical practice in inherited cardiomyopathies. Asatryan B, Medeiros-Domingo A. 2018; J Mol Med (Berl). 2018 Oct;96(10):993-1024. doi: 10.1007/s00109-018-1685-y.
- Clinical outcomes associated with sarcomere mutations in hypertrophic cardiomyopathy: a meta-analysis on 7675 individuals. Sedaghat-Hamedani F et al. Clin Res Cardiol. 2018 Jan;107(1):30-41. doi: 10.1007/s00392-017-1155-5.
Download here interesting open access manuscripts on genetics of HCM: